Blog
Is It a “Cute” Lisp, or Is It Time to See a Fort Myers Speech Therapist? The Sound-by-Age Timeline
It’s often endearing when a three-year-old announces she wants “pasketti” for dinner, or a kindergartner tells a long story in which every “r” comes out sounding like a “w.” It can also be the kind of occurrence that quietly plants a seed of curiosity in a parent’s mind: is this normal? Should something be happening by now? As Fort Myers speech therapists, we assure parents that most speech sound errors in young children are entirely typical. Children do not arrive in the world producing perfect sounds, and the journey toward clear speech follows a predictable developmental sequence.
However, it is also true that some errors do persist beyond the age when they should naturally resolve. When that happens, the earlier a child receives support, the better the outcomes tend to be.
This guide walks through the research-backed timeline of speech sound development, identifies the sounds that parents most commonly ask about (including the lisp, the “w” for “r” swap, and the elusive “th”), and explains what a Fort Myers speech therapist at FOCUS looks for when evaluating a child’s articulation.
Why some speech sound errors are developmentally normal
Your child’s Fort Myers speech therapist may explain that speech sounds are produced through an intricate coordination of the lips, tongue, teeth, palate, jaw, and airflow. Producing them accurately requires both motor learning and auditory discrimination, the ability to hear the difference between how a sound should sound and how it currently comes out. Children develop these skills gradually, and different sounds require different levels of motor precision.
The earliest sounds to emerge are those that require the least precise mouth movement: sounds like /m/, /b/, /p/, and /w/ involve the lips coming together in simple, visible movements. Later-developing sounds like /r/, /l/, /s/, and /th/ require the tongue to position itself in very specific ways that children cannot always coordinate on demand, even when they hear the sound correctly. This is why a child can hear the difference between “run” and “wun” perfectly well and still produce the second version consistently for years.
A speech sound error is considered developmentally appropriate when it is consistent with what most children that age are doing. It becomes a clinical concern when it persists significantly beyond the typical age of acquisition, or when it is affecting a child’s intelligibility, confidence, or willingness to communicate.
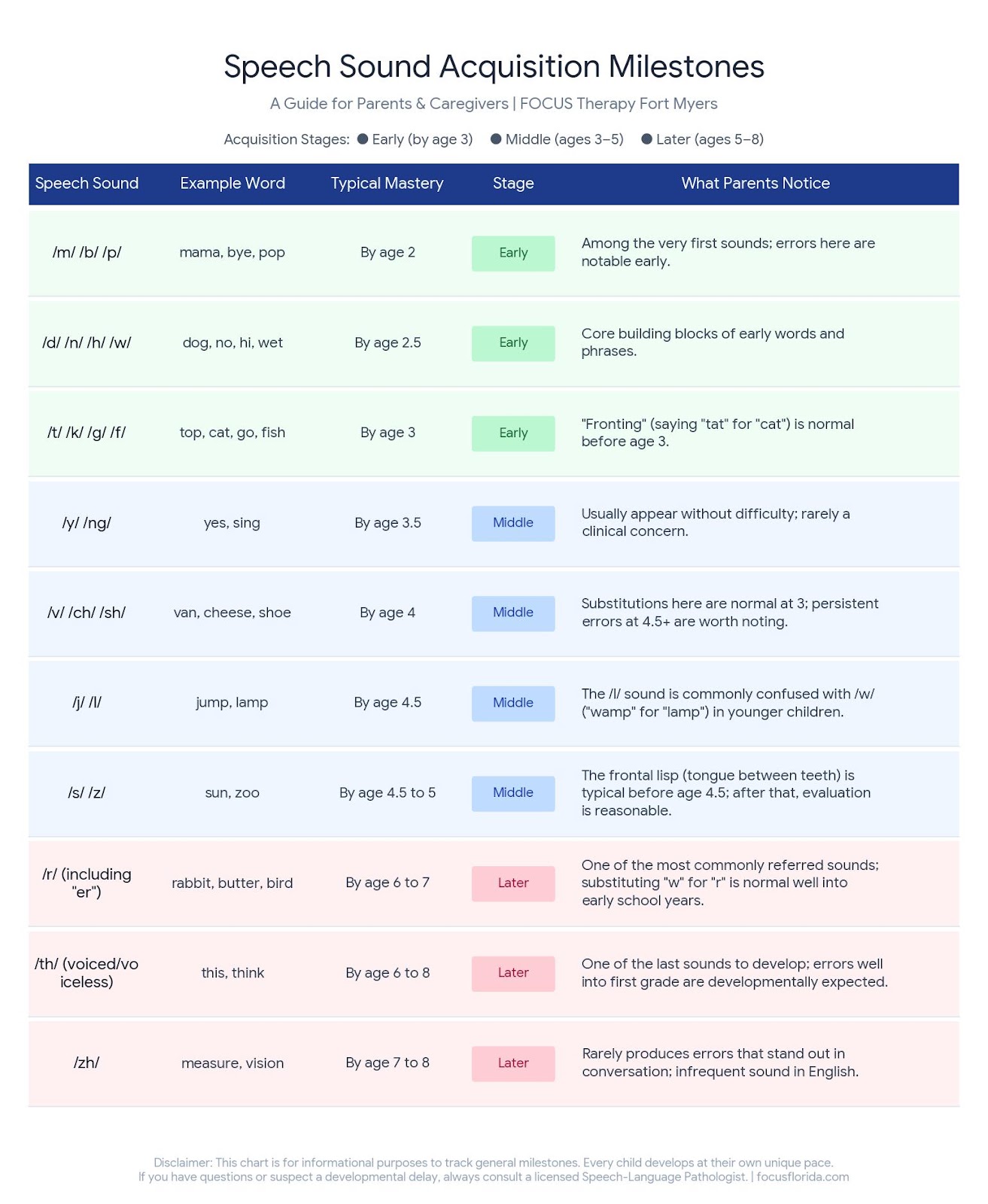
The speech sound acquisition timeline
The chart below reflects widely used norms from speech-language pathology research, including data from the landmark studies by Shriberg and McSweeny, as well as more recent normative research. Ages reflect when approximately 90% of children have mastered each sound, meaning consistent and accurate production across most contexts. Some individual variation is normal.

The speech sounds parents ask about most
The lisp: frontal vs. lateral
The word “lisp” gets used loosely to describe any distortion of the /s/ or /z/ sound, but there are actually two distinct patterns, and they have very different clinical implications.
A frontal lisp occurs when the tongue protrudes between the front teeth, producing a “th”-like sound instead of /s/. This pattern is developmentally normal in children under four to four and a half years old, because many young children are still learning to keep the tongue behind the teeth when speaking. A frontal lisp that persists past age five is worth evaluating, but it is also among the most responsive to speech therapy when addressed.
A lateral lisp is different in character. Here, air escapes over the sides of the tongue rather than straight through the center, giving /s/ and /z/ a wet or slushy quality. Unlike a frontal lisp, a lateral lisp is not a typical developmental stage at any age. When a lateral lisp is present, evaluation is generally recommended regardless of the child’s age.
The /r/ sound: why it takes so long and why it matters
The /r/ sound is one of the most acoustically complex sounds in American English and one of the most frequently misarticulated. It requires a very specific tongue body position that is largely invisible from the outside, which makes it harder for children to self-correct through imitation alone. Many children substitute /w/ for /r/ well into first and second grade, which is within normal developmental range.
By age seven, however, a persistent /r/ error begins to affect intelligibility and can become a real source of social difficulty. Children notice, other children notice, and classroom participation can be affected. The good news is that /r/ responds very well to targeted speech therapy, particularly when treatment begins between ages six and eight, before compensatory patterns become deeply established.
The /s/ and /z/ sounds: school age is the turning point
Because /s/ appears in so many English words, errors on this sound have an outsized effect on overall speech clarity. Preschool /s/ errors are expected and common. By the time a child enters kindergarten at age five, /s/ production should be mostly consistent. A child heading into first grade with significant /s/ errors is a good candidate for evaluation, particularly because reading instruction in that year leans heavily on phonological awareness of precisely these sounds.
The /th/ sound: the patient one
The /th/ sound is among the last to develop and one of the least concerning to watch and wait on. Errors on /th/ in kindergartners and even early first graders are entirely within the developmental range. Because /th/ is also relatively infrequent in English compared to sounds like /s/ or /r/, persistent errors on this sound alone rarely cause significant intelligibility problems. When /th/ errors persist past age seven or eight alongside other sound errors, they typically get addressed as part of broader articulation work.
- Categorized: Articles
What Does “Play-Based” ABA Therapy Actually Look Like at FOCUS?
When a child is referred for Fort Myers ABA therapy, parent reactions tend to fall into one of two camps. Some feel relief: finally, an evidence-based path forward. Others arrive with questions, having read message board posts, autistic adult accounts, and social media threads that gave them pause. They want to help their child and are thoughtfully weighing their options.
What our ABA therapists at FOCUS want parents to know is that the practice of ABA therapy has evolved significantly over the decades, and not every practice looks the same. There is an important history to understand, one that has shaped how the best contemporary providers approach their work, and why the field has moved toward more naturalistic, child-led models.
Here, we’re exploring what modern, play-based ABA therapy looks like in practice, how the approach at FOCUS in Fort Myers reflects that evolution, and what families can look for when evaluating any ABA provider.
Why some may approach ABA with caution
Applied behavior analysis has been around since the 1960s. In its earlier years, ABA therapy for autism often involved highly structured, therapist-directed sessions with heavy emphasis on repetition and compliance, an approach known as discrete trial training. The field looked quite different from what modern, naturalistic practices look like today.
As with many areas of clinical care, understanding has grown considerably over time. Autistic adults who experienced older models of therapy have shared valuable perspectives that have meaningfully shaped how the field approaches treatment, and those voices have been an important part of the conversation driving positive change.
The best contemporary ABA therapy practices have absorbed those lessons and evolved significantly. Most providers working in naturalistic, play-based models today are doing something that looks and feels fundamentally different from earlier approaches, and that evolution is worth understanding when families are researching their options.
Questions worth asking any Fort Myers ABA Therapy provider
- Does this program use any aversive techniques, even mild ones?
- How many hours per week is recommended, and how is that determined?
- Are goals set based on the child’s quality of life, or primarily on reducing behaviors?
- What does a typical session look like?
- How are autistic adults involved in the practice’s philosophy and oversight?
What ABA Therapy actually is: the science, simply explained
Stripped down to its foundations, applied behavior analysis is the scientific study of how behavior is learned and how it can be supported or changed. It’s based on the understanding that behavior is influenced by what happens before it (the environment, a prompt, a situation) and what happens after it (the consequence, whether something reinforcing or unreinforcing follows).
This framework is called the ABCs: antecedent, behavior, consequence. It is not inherently restrictive or clinical. It’s actually a description of how all human learning works. When a child learns that making eye contact with a parent and reaching their arms up produces being picked up and cuddled, that’s ABA principles in action. When a child learns that saying “more” gets them more of the food they love, that’s ABA. The framework itself is neutral. What matters enormously is how it’s applied, what goals are chosen, and who is directing the learning.
Fort Myers ABA Therapists
ABA is a set of learning principles, not a fixed set of techniques. Rigid, table-based drills and warm, child-led naturalistic play can both be described as “”ABA” — but they look, feel, and produce very different outcomes. The approach matters as much as the science.
The play-based approach to ABA at FOCUS

Here is the clearest way we can show you the difference between the model many parents fear and the model we practice at FOCUS Therapy:
Traditional ABA
- Therapist-directed, structured drills at a table
- Goals focused on reducing “problem” behaviors
- Compliance and imitation as primary targets
- Masking autistic traits to appear neurotypical
- Identical program regardless of the child’s interests
- High-intensity, hours-long repetitive sessions
- Success measured by behavior elimination
Play-based ABA at FOCUS Therapy
- Child-led, play-based, relationship-centered
- Goals focused on building skills and quality of life
- Communication, connection, and independence
- Supporting the whole child, not masking who they are
- Built around each child’s unique interests and strengths
- Joyful, naturally embedded learning moments
- Success measured by flourishing and functional gains
This isn’t just a philosophy statement. It changes what happens in the room every single session. And the best way to understand that is to actually picture what our sessions look like.
What a FOCUS Fort Myers ABA Therapy session actually looks like
- Categorized: ABA Therapy
- Tagged: ABA therapy, behavior therapy, Focus Therapy, Fort Myers ABA Therapy
The Parent’s Roadmap to Fort Myers ADOS Testing in Southwest Florida
The moment a pediatrician, teacher, or specialist suggests an autism evaluation, a parent’s world shifts. Even if the idea has been quietly forming in your own mind for months, even if part of you has been Googling “autism signs in toddlers” at midnight, hearing it said out loud lands differently. Suddenly there are acronyms you’ve never heard, referrals to navigate, and an overwhelming amount of information that’s hard to sort through when you’re also trying to keep life running normally.
This guide exists to take the mystery out of one specific, pivotal step: the ADOS evaluation. By the time you finish reading, you’ll know exactly what to expect, how to prepare, what the results mean, and how Fort Myers ADOS testing at a specialized practice like Focus Florida can give your family the answers and direction you need.
What the ADOS actually is — and isn’t
ADOS stands for Autism Diagnostic Observation Schedule. It’s widely considered the gold standard for autism spectrum disorder (ASD) evaluation in children and adults. When clinicians talk about “autism testing,” the ADOS is almost always part of what they mean.
The ADOS is an observational assessment, meaning it’s not a blood test, a brain scan, or a questionnaire you fill out at home. It’s a structured play-based interaction between your child and a trained clinician, designed to create natural opportunities to observe social communication, imagination, and behavior. Think of it less like a test and more like a carefully designed playdate that a specialist watches with a very specific, trained eye.

The current version
Most clinicians today use the ADOS-2, the second edition of the assessment. It has five different modules designed for different ages and language levels — from toddlers with no spoken language to verbally fluent adults. Your child will be assessed using the module most appropriate for their developmental stage, not just their age.
What the ADOS is not
It’s worth being clear about what the ADOS cannot do. It’s not a pass/fail exam. It doesn’t definitively “diagnose” autism on its own — a comprehensive autism evaluation also typically includes a developmental history interview with parents, standardized rating scales, review of previous records, and clinical judgment. The ADOS is a critical piece of that puzzle, but it’s one piece. A qualified evaluator will always look at the full picture.
The ADOS also doesn’t measure intelligence, determine your child’s “level” of autism on its own, or predict their future outcomes. It’s a diagnostic tool — its job is to help clinicians understand how your child communicates and interacts in a structured social setting, and whether those patterns are consistent with autism spectrum disorder.
The Typical Route to Fort Myers ADOS Testing
Parents come to ADOS testing through several different paths, and there’s no single “right” way to get here. Understanding the common routes can help normalize where you are in this process.
1. Pediatrician concern or referral
Your child’s doctor noticed developmental differences at a well-child visit — perhaps a speech delay, limited eye contact, or developmental screening scores that warranted a closer look. This is one of the most common starting points.
2. Early intervention or school referral
A speech therapist, early intervention specialist, or school evaluation team flagged patterns consistent with ASD and recommended a formal diagnostic evaluation to guide services and support planning.
3. Parent-initiated concern
You’ve been observing something for a while — sensory sensitivities, difficulty with social interactions, repetitive behaviors, or rigid routines — and you want answers. Families can and do self-refer for ADOS evaluations.
4. School-age recognition
Some children reach elementary school before differences become apparent — particularly girls, who often mask autistic traits more effectively. A teacher’s observation or a social-emotional struggle prompts a re-look at development.
5. Transition from a previous incomplete evaluation
Some families have been through screenings or partial evaluations elsewhere and are seeking a more comprehensive assessment, a second opinion, or an updated evaluation as their child has grown.
Wherever you’re coming from, what matters now is what happens next.

The step-by-step ADOS process: what to expect
A comprehensive autism evaluation involving the ADOS unfolds over several stages. Here’s exactly what the process looks like, from your first contact with a provider through to receiving your results.
1. Intake and scheduling
W-Sitting, Toe-Walking, and Clumsiness: Fort Myers Occupational Therapists Red Flags
Your four-year-old is playing on the living room floor and you notice they’re sitting in that strange position again, legs splayed out behind them like a letter W, while their sibling sits cross-legged. Or maybe your son has been walking on his tiptoes since he started walking, and everyone keeps telling you he’ll grow out of it. Or perhaps your daughter trips over her own feet so often that she’s become the kid who always has a scraped knee. As Fort Myers occupational therapists, we want parents to know they’re right to pay attention, trust their gut, and ask for an outside opinion when something seems off. Many of these “physical quirks are among the earliest, “quirks” are among the earliest and most visible signs that a child’s sensory or motor development could use some support. The good news is that with early intervention through pediatric occupational therapy, some of these concerns can be addressed entirely before school readiness is affected.
What is W-sitting and why do kids do it?
W-sitting happens when a child sits on the floor with their bottom on the ground, knees bent forward, and both feet pointing outward on either side of their hips. If you looked down from above, their legs form the shape of a capital W. It’s surprisingly common in toddlers and preschoolers, and sometimes it’s a child’s default to this position because it actually feels stable and comfortable.
The problem has less to do with the sitting itself and more with the fact that it can be a warning sign. Children gravitate toward W-sitting because it creates a wide base without requiring their core muscles to work. It’s essentially a cheat code around core stability. When children don’t develop core strength and trunk control properly, their bodies find a mechanical workaround — and W-sitting is one of the most common ones.

Why it matters beyond just posture
Short-term W-sitting isn’t dangerous. But children who habitually sit this way may develop real concerns over time — tightening of hip muscles and tendons (particularly the hip flexors and internal rotators), reduced balance and core strength, and difficulty with the rotation movements that are essential for tasks like crossing the midline of the body.
Crossing the midline — reaching your right hand to the left side of your body, or vice versa — is something we take for granted as adults, but it’s a crucial developmental milestone. It underpins handwriting, sports coordination, and even the ability to read a page left to right. Children who W-sit excessively may avoid or struggle with these crossing movements without anyone connecting the dots.
When to pay attention
Occasional W-sitting in toddlers is normal. It becomes a concern when a child only sits this way, resists being repositioned, or is over age 4–5 and still defaulting to this position exclusively. If you notice it paired with clumsiness, delayed milestones, or low muscle tone, that’s a stronger signal.
What to try at home
You can gently encourage better sitting habits by reminding your child to sit “criss-cross applesauce” or in a side-sit position, and by building core strength through play (think obstacle courses, crawling games, and activities that challenge balance). But if W-sitting is the overwhelming preference and your child resists alternatives, an occupational therapy evaluation can identify whether an underlying sensory or motor issue is driving the behavior.
Toe-walking: habit, phase, or hidden signal?
Nearly every toddler goes through a toe-walking phase. When children are first learning to walk, walking on their tiptoes is normal and expected — it’s part of experimenting with movement. Most children transition to heel-toe walking naturally by the time they’re 2 or 3 years old.
When toe-walking persists past age 3, and especially past age 4, parents are right to take a closer look. Persistent toe-walking — sometimes called “habitual toe-walking” or “idiopathic toe-walking” — is one of the most Googled childhood physical concerns for a reason: it’s common, it’s visible, and it has a wide range of possible causes.

Why kids toe-walk: the full picture
There’s no single reason children continue to toe-walk. Some causes are structural (a shortened Achilles tendon or tight calf muscles can physically make flat-footed walking uncomfortable). Other causes are neurological, since conditions like cerebral palsy and hereditary spastic paraplegia can affect gait. And increasingly, occupational therapists are identifying sensory processing differences as a major driver.
The 2026 Summer “Regression” Prevention Guide from our Fort Myers ABA Therapists
School ends, the schedule dissolves, and within few weeks (sometimes a few days, if we’re honest) you start noticing your child’s skillsets slipping. The morning routine that finally felt manageable becomes a battle again. The words your child had been using more consistently start fading back. The meltdowns that had decreased in frequency tick back up.
This is called summer regression, and it is real, it is common, and the good news is it is largely preventable.
Most people have heard of the academic “summer slide,” the research-backed finding that children lose a measurable portion of their school-year learning over summer break. What fewer people realize is that children receiving behavioral and developmental therapy experience an entirely parallel phenomenon. Social skills, communication patterns, self-regulation strategies, daily living routines: these are all skills that require ongoing practice and structured reinforcement to maintain. When that structure disappears for ten or twelve weeks, the skills don’t just pause. They can actually erode.
At FOCUS Therapy, our Fort Myers ABA therapists sees this every fall. And we’ve spent years helping families understand how to avoid it.
Why Summer Is Uniquely Challenging for Children with Autism and Developmental Differences

Children who receive ABA therapy, speech therapy, and occupational therapy have typically made their progress through something consistent: structure, repetition, reinforcement, and a predictable environment where expectations are clear.
Summer break can have a big impact on that consistency.
The routine changes. The people change. The expectations change. For many children, particularly those with autism spectrum disorder, this level of disruption doesn’t feel like freedom. It feels like chaos. And when a nervous system is dysregulated and the familiar cues for expected behavior disappear, skills that were emerging or recently mastered become unreliable.
- Categorized: ABA Therapy
- Tagged: ABA therapy, Fort Myers ABA therapists, Fort Myers ABA Therapy
Gestalt Language Processing: Why “Repeating Movie Lines” Is Actually Progress
Your child doesn’t ask for juice. Instead, they look at you and say, “To infinity and beyond!”
Or maybe they recite an entire scene from their favorite show when they’re excited. Or when you ask “How are you?” they respond with a phrase you vaguely recognize from a cartoon they watched six months ago.
If this sounds familiar, you may have already stumbled across the term Gestalt Language Processing — or heard someone mention echolalia at a doctor’s appointment. And if you’ve spent any time in parent groups or Fort Myers speech therapy circles in the last few years, you know that this topic is everywhere right now.
There’s a reason for that. A lot of what we once misunderstood about how some children acquire language is being looked at with fresh eyes. And for parents who have been quietly puzzled or worried by their child’s scripted speech, the conversation happening in Fort Myers speech therapy offices and across the field is genuinely encouraging.
Here’s what you actually need to know.
What Is Gestalt Language Processing?
To understand Gestalt Language Processing (GLP), it helps to first understand that not all children learn language the same way.
Most children build language the way you might imagine: one word at a time. They say “mama,” then “ball,” then “more,” then “want ball,” gradually assembling language piece by piece. This is called analytic language development.
But some children, particularly many autistic children, though not exclusively, take a different route. Instead of starting with single words, they absorb and reproduce entire chunks of language all at once. A phrase from a movie. A line from a book. A sentence they heard a parent say repeatedly. These “chunks” are called gestalts, and the children who learn this way are increasingly described as Gestalt Language Processors.
The idea that children develop language through these gestalt-style chunks isn’t new. ASHA, the American Speech-Language-Hearing Association, acknowledges on its Practice Portal that gestalt language acquisition is “a style of language development with predictable stages that begins with production of multi-word gestalt forms and ends with production of novel utterances.” In other words, the scripted phrases your child repeats aren’t random noise. They are, for many children, the first rung of a very real developmental ladder.
You can read ASHA’s guidance on echolalia and gestalt language acquisition directly here: https://www.asha.org/Practice-Portal/Clinical-Topics/Autism/Echolalia-and-Its-Role-in-Gestalt-Language-Acquisition/
What Echolalia Actually Is (and Isn’t)
Echolalia is the repetition of words or phrases heard from others. It gets a bad reputation, largely because it used to be framed as a behavior to extinguish. But research has been shifting that picture significantly.
A growing body of evidence, cited by ASHA, has identified a wide range of communicative functions that echolalia actually serves: turn-taking, labeling, requesting, affirming, and protesting, among others. When your child says “To infinity and beyond!” in response to something exciting, they may be expressing enthusiasm or celebration. When they repeat a phrase from a show about a character being scared, they may be telling you they’re scared. The script is their word for the feeling.
This is not meaningless behavior. For many children, it is the most sophisticated communication they have available to them right now, and the evidence increasingly supports treating it that way.
It is worth being honest with you: the term “Gestalt Language Processing” and the specific therapy protocol built around it are still areas of active research and professional discussion. The science of echolalia is robust. The specific frameworks for identifying and treating GLPs are still being studied and refined. At FOCUS Therapy, we pay close attention to this distinction, which is why our approach is grounded in what the evidence strongly supports: meeting your child in their language, and helping them build from there.
The Stages: From Scripts to Self-Generated Language

One of the most useful things to understand about children who use scripted speech is that there is a developmental arc to it. These stages have been described in the clinical literature and referenced in ASHA’s practice guidance:
In the earliest stage, a child produces whole, unanalyzed phrases. Think of the movie line delivered perfectly, context and all. This is communication. It may not look like what we’re used to, but it is your child using the tools they have.
- Categorized: Speech Therapy
- Tagged: Fort Myers speech therapy, speech therapists, speech therapy
The “Whole-Child” Evaluation: Why We Might Suggest Multiple Therapies After Fort Myers ADOS Testing
Whatever brought you to our doors for Fort Myers ADOS testing, whether it was a teacher’s suggestion or your own sense that your child wasn’t keeping pace with their peers, you were focused on one thing: getting answers.
Now, you have some answers — and recommendations for multiple pediatric therapies, possibly including speech therapy, occupational therapy, and ABA therapy.
For many parents, that moment can feel overwhelming. Our hope here is to offer some further insights on why we often recommend multiple therapies after your child’s Fort Myers ADOS test has been fully assessed.
First: What Is ADOS Testing, and What Does It Actually Tell Us?
ADOS stands for the Autism Diagnostic Observation Schedule. The current version, the ADOS-2, is widely considered the gold standard diagnostic tool for autism spectrum disorder (ASD). It’s a structured, play-based assessment administered by a trained clinician who observes your child’s social communication, language, and behavior in real time. It’s not a questionnaire. It’s not a checklist. It’s a careful, standardized window into how your child actually engages with the world.
What the ADOS helps to get diagnosis — or a ruling out of one. What it does not give us, on its own, is a complete picture of everything your child needs. That’s where the “whole-child evaluation” comes in.
The Report Said “Autism.” Now What?
A diagnosis, whether it’s ASD, developmental delay, or another finding, is the beginning of a conversation, not the end of one. And that conversation has to go deeper than a single label.
Here’s why: autism (and many other developmental profiles) isn’t one thing. It’s a constellation. Two children can carry the same diagnosis and look completely different in a therapy room. One child might be highly verbal but struggle to read social cues. Another might have almost no expressive language but rich emotional awareness. A third might have significant sensory sensitivities driving behaviors that, on the surface, look purely behavioral.
The American Academy of Pediatrics (AAP) is explicit about this: after an ASD diagnosis is made, the AAP recommends that a multidisciplinary team characterize the full scope of a child’s needs — including formal cognitive and language assessments, as well as occupational therapy, audiology, and visual assessments. In other words, the diagnosis is just the starting line.
This is exactly how we think about evaluation at FOCUS Therapy, and it shapes every recommendation we make after Fort Myers ADOS testing.

Why a “Behavior Problem” Is Often Different Things at Once
Let’s walk through a scenario that plays out in our clinic regularly.
A parent comes to us concerned about their child’s meltdowns, noncompliance at school, and aggressive behavior toward siblings. On the surface, this sounds like a behavior issue, so ABA therapy will likely be part of the picture. But when we look closer, here’s what we often find:
The “behavior” is actually sensory dysregulation. The child who flips the table at lunch isn’t being defiant — they’re overwhelmed. The noise of the cafeteria, the texture of their clothing, the brightness of the lights. Their nervous system is in overdrive, and the meltdown is a pressure release valve. This is a sensory processing issue, and it calls for occupational therapy with a sensory integration focus, not just behavioral intervention.
The “behavior” is actually a communication breakdown. A child who hits when frustrated often does so because hitting works faster than words. They don’t yet have the language tools to say “I’m overwhelmed” or “I don’t understand what you’re asking me.” Once a speech-language pathologist helps build those tools, the hitting often decreases — not because a behavior was extinguished, but because the child now has a better option. That’s the work of speech therapy.
The “behavior” is also a behavioral pattern that needs direct intervention. After we’ve addressed the sensory and communication layers, there are still learned behaviors: escape behaviors, attention-seeking patterns, rigid routines. ABA can help tremendously in treating these issues, but it works better, faster, and more durably when the child isn’t simultaneously flooded by sensory input they can’t process, or frustrated by an inability to express their needs.
This is why our team looks at all three together.
What “Silo-Free” Care Actually Looks Like
- Categorized: ADOS Testing
- Tagged: ADOS testing, Fort Myers ABA Therapy, Fort Myers ADOS, Fort Myers ADOS testing
The Power of “Wait Time”: A Simple Speech Therapy Hack For Parents
Your child is standing in front of the snack cabinet, clearly wanting something. You ask, “What do you want?” Then before they’ve had even a second to think, you follow up with, “Do you want crackers? Or the pretzels? Here, I’ll just grab the crackers.”
It’s one of the most natural things parents do. But as it turns out, one of the most common habits our Fort Myers speech therapy team at FOCUS Therapy gently encourages families to change.
The good news is the fix is simple, free, and you can start using it today. It’s called wait time — and it’s one of the most powerful tools in the Fort Myers speech therapy toolkit.
What Is “Wait Time,” Exactly?
Wait time (sometimes called an “expectant pause”) is exactly what it sounds like: after you speak to your child, you pause and wait, anywhere from 5 to 10 seconds, giving them the opportunity to initiate or respond before you step in.
That might not sound like much. But those few seconds of silence? They’re doing a lot of heavy lifting.

Why Silence Is So Powerful
Here’s the thing most parents don’t realize: children, especially those with speech or language delays, need significantly more time to process language than adults do. Our conversations as grown-ups move fast. We expect quick back-and-forth. But for a child whose brain is still building the connections needed to understand what was said, formulate a response, and produce speech, that typical conversational pace can feel like trying to answer a question while someone is already asking the next one.
When you pause and wait, you’re giving your child’s brain the runway it needs to actually land.
The American Speech-Language-Hearing Association (ASHA), which is the gold standard professional organization for speech-language pathologists, specifically recommends that parents “pause after speaking” to give children a chance to respond, noting that this is one of the most effective everyday strategies for supporting speech and language development.
Research in educational settings backs this up powerfully: when adults wait just 3 to 5 seconds after asking a question, children give longer, more accurate responses, and more of them volunteer to communicate at all. Imagine what 5 to 10 seconds can do.
The Real Magic: Encouraging Initiation
Beyond helping kids respond, wait time does something even more exciting — it encourages children to initiate communication on their own. This is huge.
In speech therapy, we distinguish between a child who communicates when prompted and a child who starts the conversation themselves. That second skill — initiation — is a major developmental milestone, and it’s something we work on every single session.
When you consistently pause and wait, you’re creating space for your child to take the first turn. Instead of you always being the one to label, request, or comment, your child gets the chance to lead. Over time, this builds not just vocabulary and sentence structure, but communicative confidence.
How to Do It: Your 5-Step “Wait Time” How-To
Ready to try it? Here’s how our Fort Myers speech therapy team recommends putting wait time into practice at home:
- Categorized: Speech Therapy
- Tagged: Fort Myers speech therapy, speech therapy
Lee County School IEPs in 2026: What Parents Need to Know about Fort Myers IEP Planning — and How FOCUS Therapy Can Help
If your child has an Individualized Education Program (IEP) through the Lee County School District, you are navigating one of the most important and complex aspects of raising a child with a disability or developmental difference. You are also doing so during a year of significant change, both in how the district delivers services and in the state-level scholarship landscape that affects how families can fund private therapy. Here, we’re offering a bit of insight into what is happening, what it means for your child, and a few ways FOCUS Therapy can help support your child’s academic journey.
What Is Happening in Lee County Schools Right Now
In 2025, an independent audit of the Lee County School District’s Exceptional Student Education (ESE) program flagged some concerns, with two areas in particular requiring immediate attention: the development and delivery of ESE services and accommodations, and ESE delivery consistency and maturity. A review of 40 IEPs identified 467 services and accommodations that were not being consistently delivered or documented. In response, the district launched a centralized dashboard system to track IEP services in real time.
More recently, in March 2026, the district announced a significant structural change: a shift to a “cluster school model” for ESE service delivery. This means some students with disabilities will be reassigned to different schools, ones designated to serve their specific needs, rather than receiving services at their home school. The district’s stated goal is to enhance student outcomes, better support ESE staff, and address a teacher shortage that is, in their own words, “acutely impacting the ability to meet demands.”
For many families, that’s going to mean a new school, a new routine, and likely more than a few questions.
The Family Empowerment Scholarship: What It Means for Your Family
Florida’s Family Empowerment Scholarship for Students with Unique Abilities (FES-UA), administered through Step Up For Students, is one of the most powerful (and underutilized) tools available to Lee County families of children with disabilities. Established under Florida law (Section 1002.394, Florida Statutes) and expanded significantly by HB 1 in 2023, the FES-UA provides eligible families with an Education Savings Account averaging approximately $10,000 per year, and up to $22,000 to $34,000 annually for students with the highest levels of need.
Critically, those funds can be used for private therapies, including speech-language pathology, occupational therapy, and ABA therapy, in addition to private school tuition, tutoring, curriculum, and other approved educational expenses. Students are eligible if they have a current IEP issued by a Florida school district or a qualifying diagnosis from a licensed physician or psychologist. Children as young as 3-years-old can qualify.
One important thing families must understand: students who choose to access the ESA option of FES-UA cannot simultaneously remain enrolled in a Florida public school. This is a big decision that affects your child’s IEP rights and school-based services. It is not the right choice for every family. But for some, it opens meaningful access to private therapeutic services that might otherwise be out of reach financially.
Applications for the 2026–27 school year opened February 1, 2026, with a priority renewal deadline of April 30, 2026. If you have not yet explored this scholarship for your child, we encourage you to visit stepupforstudents.org to learn whether your family qualifies.

Where FOCUS Therapy Fits In
FOCUS Therapy does not provide school-based services — and we want to be clear about that distinction, because it matters legally and practically. What we do provide is private therapy services complementary to what your child receives at school. While there are wonderful, dedicated school-based therapy providers throughout Southwest Florida, the reality is they are also grappling with sizable caseloads, staffing shortages, and the inherent limitations of a school environment.
New to FOCUS Therapy? Here’s What You Need to Know!
Welcome to the FOCUS family! Whether your child has just received their first evaluation recommendation, you’re transferring from another clinic, or you’re simply exploring your options in Southwest Florida: We are genuinely glad you are here! Starting or changing your pediatric therapy journey can feel overwhelming. There are new faces, new routines, new terminology, and sometimes more questions than answers. Our goal is to make this transition as smooth, clear, and encouraging as possible. So before your first appointment, here are a few things to know about getting started at FOCUS Therapy.
Who We Are
FOCUS Therapy is a pediatric therapy clinic located at 4997 Royal Gulf Circle in Fort Myers, Florida, open Monday through Friday from 7 a.m. to 6 p.m., with Saturday appointments available by arrangement. We serve children throughout Lee County and surrounding communities in Southwest Florida, including Cape Coral, Lehigh Acres, Bonita Springs, Estero, and Naples.
FOCUS stands for Follow Our Course Until Successful — and that is not just a motto. It is our commitment to our patients and our promise to their parents and caregivers. Accomplishments may not happen overnight, but breakthroughs happen here every day. Our therapists are dedicated to the journey, and you and your child become part of our FOCUS family from day one.
What We Offer
FOCUS is a multidisciplinary clinic. This means we bring several therapy disciplines together under one roof.
Our services include:
Speech & Language Therapy, which helps children develop communication skills — articulation, language comprehension and expression, social communication, and more. Approximately 75% of children ages 2 and 3 who enter pediatric therapy do so because of a speech or language delay. If your child is not yet meeting developmental milestones for their age, a speech evaluation is a great first step.
Occupational Therapy (OT), which focuses on building the skills children need for daily life — fine motor coordination, sensory processing, self-care routines, and the ability to participate meaningfully in home, school, and social settings.
ABA / Behavior Therapy, which uses evidence-based principles of learning and positive reinforcement to help children develop socially significant behaviors, reduce challenging behaviors, and build independence. ABA is most commonly used with children on the autism spectrum, but the principles apply broadly. Our team starts with a thorough assessment to understand the function of each behavior before creating an individualized plan.
Feeding Therapy, which supports children who struggle with eating, swallowing, or food aversions — a more common challenge than many families realize, and one that can significantly affect nutrition, growth, and mealtime quality of life.
Teletherapy, which is available on a limited bases for some speech and occupational therapy services. The option depends on the therapist and also the patient. It may not be the best for every child or family, but it sometimes allows us to reach families who cannot access in-clinic care. Sometimes it helps with minimizing missed appointments if the patient or any of their household members have a contagious illness. Talk to our office staff or your child’s individual therapist(s) if this is something you want to explore.

Beyond direct therapy services, FOCUS Therapy also offers ADOS Testing for autism and some specialized services to help support parents and families on this journey.
ADOS Testing — the Autism Diagnostic Observation Schedule — is the gold-standard diagnostic tool for assessing autism spectrum disorder. FOCUS has been a leading provider of ADOS testing in Fort Myers since 2019, and we are able to assess children as young as 18 months. An early diagnosis, followed by early intervention, is consistently associated with the best long-term outcomes for children with autism.
Behavior Consulting is available for families whose child struggles with defiance, aggression, tantrums, or social challenges, but who does not have a qualifying diagnosis for ABA therapy. It also offered to families of children who may be on a waitlist for ABA Therapy (at our clinic or elsewhere) who could use some help creating a behavior plan to help bridge the gap before therapy starts. Our board-certified behavior analysts work directly with parents to understand the root of the behavior and develop a practical, evidence-based plan. Behavior consulting does not require a diagnosis, is self-pay, and it can be provided in-clinic, in-home, by phone, or via video conference.
IEP Assistance and Planning is one of the most meaningful — and underutilized — services we offer. IEP meetings can feel intimidating. Parents often walk in unsure of their rights or how to advocate effectively for their child. Our team, led by FOCUS Founder Jennifer Voltz-Ronco, MS-CCC/SLP — a former school-based speech therapist — can help you prepare for your child’s IEP meeting and even attend alongside you to advocate for the services and accommodations your child needs and deserves.
What to Know Before You Arrive
- Categorized: FOCUS News
- Tagged: Focus Therapy, Fort Myers ABA Therapy, Fort Myers occupational therapy, Fort Myers speech therapy, speech therapists