behavior therapy
What Does “Play-Based” ABA Therapy Actually Look Like at FOCUS?
When a child is referred for Fort Myers ABA therapy, parent reactions tend to fall into one of two camps. Some feel relief: finally, an evidence-based path forward. Others arrive with questions, having read message board posts, autistic adult accounts,…
- Categorized: ABA Therapy
- Tagged: ABA therapy, behavior therapy, Focus Therapy, Fort Myers ABA Therapy
The “Playdate Playbook”: How to Facilitate a Successful Home Playdate for a Child with Social Communication Delays
For many parents, organizing a playdate seems like second nature—invite a friend over, let the kids play, and supervise from the sidelines. But for parents of children with social communication delays, including those with autism spectrum disorder (ASD), ADHD, or…
- Categorized: ABA Therapy
- Tagged: ABA therapy, behavior therapy, Fort Myers ABA Therapy
Managing Therapy Schedules: Tips for Busy Southwest Florida Families
Juggling therapy appointments alongside work, school, extracurriculars, and family life can feel overwhelming for Southwest Florida families. Between tourist traffic on US-41, severe weather, and the the constant hustle of daily life for parents with young children, our Fort Myers…
- Categorized: ABA Therapy
- Tagged: ABA therapy, behavior therapy, Fort Myers ABA Therapy
It’s Not Just a Tantrum: Fort Myers ABA Therapists Offer 4 Reasons Your Child Does What They Do (and How to Respond)
Our Fort Myers ABA therapists at FOCUS Therapy recognize there are few things more challenging than watching your child melt down in the middle of the grocery store, refuse to get dressed for school, or repeatedly engage in behaviors that…
- Categorized: ABA Therapy
- Tagged: ABA therapy, behavior therapy, Fort Myers ABA Therapy
10 Questions Parents Should Ask Their Child’s FOCUS Therapy Team
As a parent, you are your child’s most important advocate. When your child begins therapy—whether it’s occupational therapy, speech therapy, ABA therapy or a combination of services—you’re entering into a partnership with professionals who are here to support your family’s…
Behavior Consulting Empowers Parents & Improves Family Routines
Parenting comes with its share of beautiful moments and challenging days. Whether you’re navigating bedtime battles, mealtime struggles, or simply trying to establish consistent routines that work for your family, you’re not alone. At FOCUS Therapy in Fort Myers, we…
- Categorized: ABA Therapy, Behavior Consulting, Behavior Therapy
- Tagged: ABA therapy, behavior consulting, behavior interventions Fort Myers, behavior therapy, Fort Myers ABA, Fort Myers ABA Therapy, Fort Myers BCBA, Fort Myers behavior consulting, Fort Myers parent coaching, parenting help Fort Myers
Best Fort Myers Playgrounds and Parks for Sensory-Friendly Play
As Fort Myers occupational therapists who work with many families, we know how challenging it can be to find the perfect playground where your child can thrive. Whether your little one is sensory-seeking, sensory-avoiding, or somewhere in between, finding spaces…
Building Routines: Fort Myers Parent Coaching Teaches Consistency for Kids Who Need Predictability
For many children, particularly those with developmental differences, autism spectrum disorder, ADHD, or sensory processing challenges, predictability isn’t just preferable—it’s essential. At FOCUS Therapy, our Board Certified Behavior Analysts (BCBAs) work closely with parents receiving our Fort Myers parent coaching…
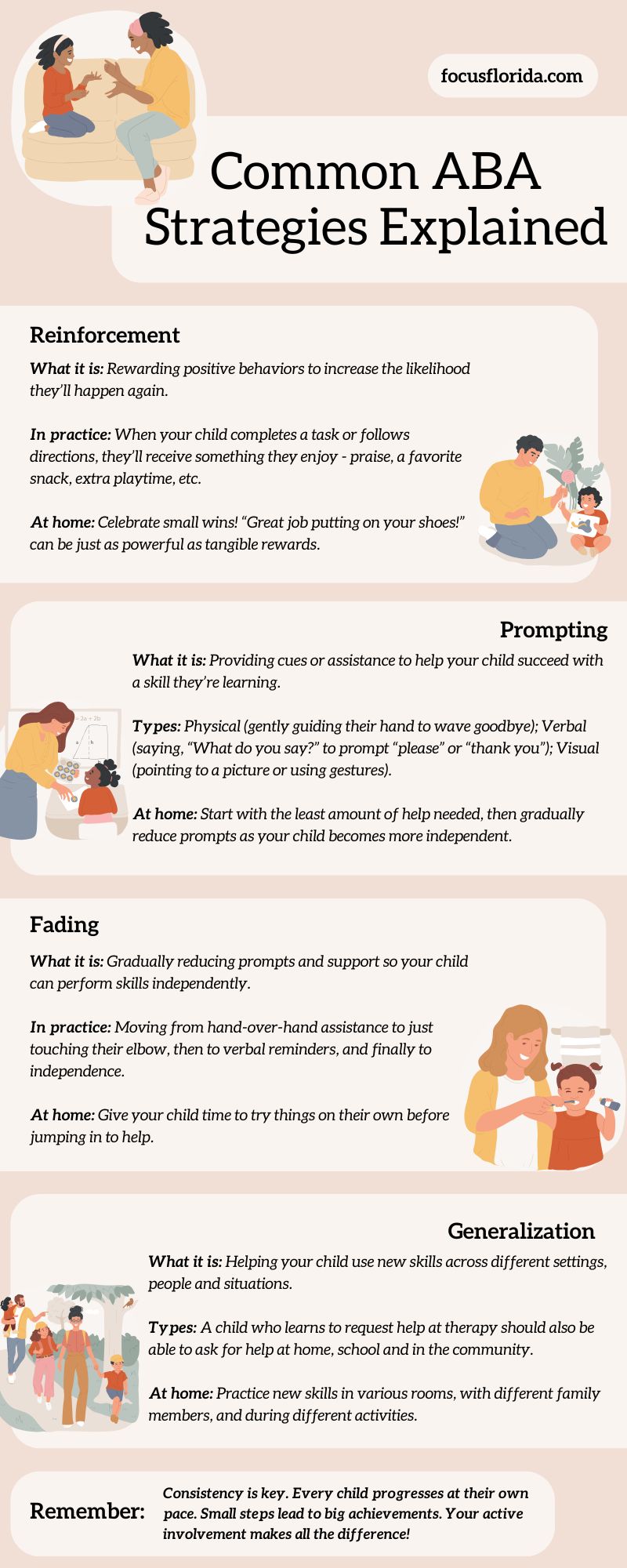
Common Fort Myers ABA Therapy Strategies
Questions about your child’s behavior therapy? The Fort Myers ABA therapy team at FOCUS is here to support you every step of the way. FOCUS Therapy offers Fort Myers ABA therapy, occupational therapy, speech therapy, parent coaching, IEP assistance and…
- Categorized: Behavior Therapy
- Tagged: ABA therapy, behavior therapy, Focus Therapy, Fort Myers ABA Therapy
Collaborative Approaches: How Fort Myers ABA Works With Other Therapies
At FOCUS Therapy in Fort Myers, we believe that the most effective approach to pediatric therapy isn’t found in isolated treatment, but through thoughtful collaboration between disciplines. Our multidisciplinary model combines Fort Myers ABA (Applied Behavior Analysis), Speech-Language Therapy, and…